Duncan’s Story
Duncan had a big personality long before we met him.
I received Duncan’s diagnosis during my 14-week checkup, my Nuchal Translucency (NT) Scan. I went to the appointment alone out of habit; our 1.5-year-old son, Finnegan, was born in 2021 during the pandemic so I was used to going by myself while my husband, Trevor, was at work. I figured it was business as usual since my bloodwork came back fine. I jokingly (but serious) said to the technician, “everything look good?!” Also, out of habit, and fear due to a miscarriage in early 2020 before having Finnegan, I started asking this at all my ultrasounds. The technician only responded by saying, “the doctor will be right in”. I knew something was wrong. I waited 30 minutes for the doctor to come see me and do his own scan. We went back to the doctor’s office, and he asked me all sorts of questions about my health, my age, our son, my miscarriage. Then he asked, “do you have any reason to believe this pregnancy will be any different than your previous?” This is when he explained that what they were seeing was Duncan’s diaphragm hadn’t closed like it was supposed to for 14 weeks. He said it was called Congenital Diaphragmatic Hernia; his diaphragm didn’t close which would allow his organs to move into his chest. He wanted me to come back at 16 weeks just to double check. I cried in the car the whole way home, sobbing to my husband on the phone. The doctor mentioned that if this was indeed what Duncan had, then we would be officially diagnosed and treated at CHOP. I looked it up on their website. It was the only rabbit hole I let myself go down. At 16 weeks pregnant, April of 2022, the maternal fetal medical doctor at my primary hospital confirmed the diagnosis.
At 21 weeks I had my first of what seemed like 100 appointments at CHOP. After an MRI, a detailed ultrasound, echocardiogram, and genetic counseling, the surgeon and maternal fetal medical doctors told us that Duncan had CDH on the left side (LCDH). There was a tiny portion of his liver that had come through the hernia, and this was almost best-case scenario. The severity of his diagnosis was considered “moderate”. They estimated he would have surgery to repair the hernia about one week after he was born, and he would be in the NICU for a few months, likely to be home around Christmas.
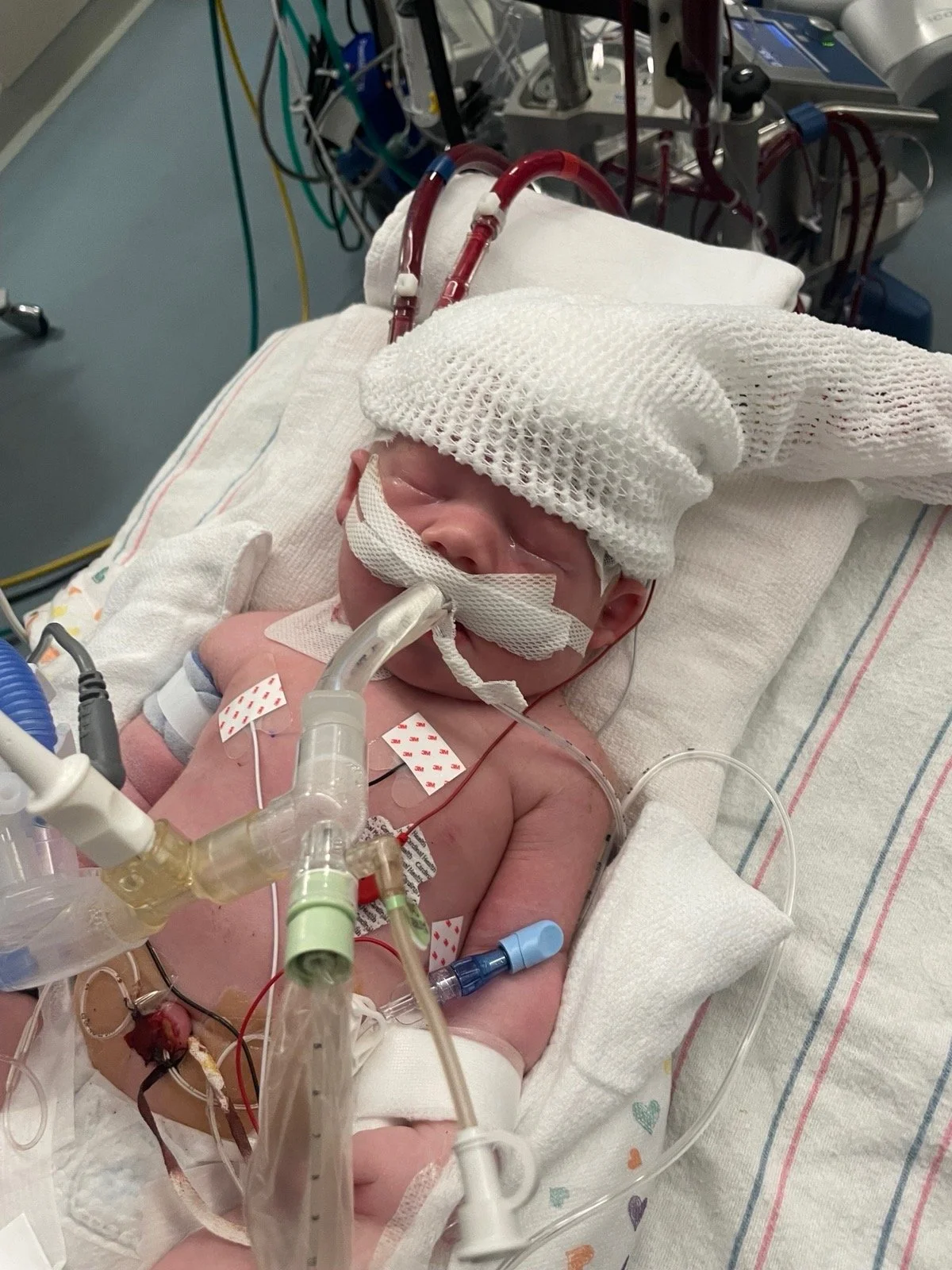
Time seemed to move so slowly that summer, but Duncan was growing so well, and I was getting bigger each day with amniotic fluid. All his scans were beautiful; he was doing great. I was considered high risk before even receiving Duncan’s diagnosis, due to my age and hypertension. I had to deliver our oldest son a few weeks early due to my blood pressure, so our goal was to do whatever it took to get Duncan to full term to give his lungs the best chance possible. We scheduled my c-section at CHOP for Wednesday, September 21st. I went in to have my blood pressure checked on Friday, September 16th and it was too high, so they induced me that day. I remember crying so hard to our doctor, I wasn’t ready yet, he wasn’t ready yet. He was the safest he would ever be in my belly. Duncan was delivered covered in meconium, we don’t know why, and this had a huge impact on his already weakened lungs. The doctors treated him for the infection, and he was doing fine. Just a couple of hours later, while my husband had quickly run home to get our bags, the neonatologists came to my room and told me that Duncan had taken a very serious turn for the worse and we needed to put him on ECMO to save his life. His heart was much weaker than anyone had anticipated. ECMO ended up causing him to have brain bleeds and seizures, so we had to make the difficult decision to take him off this highest form of life support.
We shared our special moments with him; he got to meet his brother and extended family. We washed his hair; he had the most beautiful head of red hair. The medical team expected he would only live about 10 minutes or so after taking him off ECMO, but he held on for another 12 hours. As we watched all the monitors and tracked his heart rate, Trevor and I both thought that maybe, just maybe, Duncan would pull through. But we knew that even if there was some miracle and he survived, it would be at what cost? We couldn’t hold Duncan while he was still hooked up to all the machines. The nurses told us to let them know when we were ready to hold him, that would mean taking him off everything, and I asked them to just tell us when it was time. Trevor and I fell asleep on Sunday, September 18th, at Duncan’s bedside, and woke up the next morning to the nurse telling us it was time to hold him. The nurses unplugged everything and gently put Duncan in my arms, and I sobbed and smiled looking at him, holding him for the first time. He was a big boy - 8 lbs, 8 oz, the biggest in the NICU. He passed away peacefully in our arms in the early morning hours of Monday, September 19th, after 3 days of fighting with all his might.
Duncan is a gift in our lives, and we talk about him every day. His older brother, Finnegan, and younger sister, Fiona, will grow up knowing that he was a warrior and fought bravely, and now his mission is to help other CDH babies and families and hopefully find an end to this birth defect.